The 5 Electronic Progress Notes Tools Your Small Practice Needs
As more mental health care providers realize the value of electronic progress notes, it’s helpful to take a closer look at the specific capabilities that make them work well.
A well-structured electronic progress note solution is critical when it comes to determining whether patients are improving over time, so it’s essential to keep concise, yet comprehensive, progress notes during each patient encounter.
This not only helps providers monitor care delivery, but also ensures notes are sufficiently clear to any third parties that are approved to access them.
Whether you already own a therapy progress notes software or you’re evaluating multiple systems for a new purchase, this article will prove useful. We’ll break down why progress note software is beneficial, and then explain the tools you need to optimize progress notes for mental health to get the most value from them.
Benefits of Progress Notes Software Templates
For the above reasons, mental and behavioral health care providers must optimize their progress notes templates and layouts to create the best documentation possible in the most efficient way. Doing so can bring the following benefits:
Better patient insights. Progress notes experts advise physicians to include all the relevant information related to patients and also include plans for next sessions. With software, it’s possible to customize progress notes templates to ensure every note is both streamlined and complete.
Improved care delivery. If all clinicians in a practice are capturing the same amount of patient data in the same way, it’s possible to generate meaningful reports about care quality in the organization.
Increased productivity. Notes templates with time-saving functions (e.g., pre-populated menus) can expedite data entry, allowing you to see more patients per day.
To help you achieve these results, electronic health records (EHR) vendors offer several different data-entry tools in their solutions. These tools make creating electronic progress notes faster and easier:
The Top 5 Tools for Optimizing Electronic Progress Notes

Depending on the design and flexibility of individual EHR solutions, users often have the ability to choose how they want each of these tools incorporated in their practice’s progress notes templates. The level of customization offered (and whether this comes at an additional cost) may vary among different products.
Electronic Progress Notes Tools in Action
Below are some real-life examples that show how each tool can be used to optimize a progress note for mental health care providers. The software vendors showcased offer most, if not all, of these tools:
Narrative Note Buttons
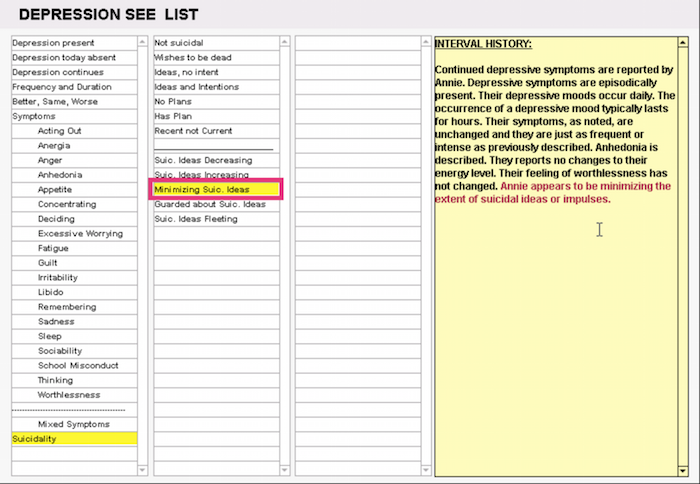

ICANotes Behavioral Health EHR
HOW IT WORKS: Narrative note buttons are clickable boxes of descriptive text. These automatically generate a narrative description of a patient’s symptoms or behaviors in the order those boxes are selected by the user.
Narrative note buttons can be implemented in certain assessment portions of the patient’s progress note, eliminating the need for manual typing.
In the screenshot above, a psychotherapist is documenting the interval history of a fictional patient (Annie) by selecting symptom information from a list. On the left, we can see two boxes highlighted “Suicidality” and “Minimizing Suic. Ideas.”
When the user selects those highlighted buttons, the software generates the red sentence in the note on the right that reads, “Annie appears to be minimizing the extent of suicidal ideas or impulses.”
KEY BENEFITS: This tool is best used in any part of your note requiring a description that can be templated to save time. For example, common observations about symptom presence, duration and frequency can be chosen from a comprehensive list of answer options.
Drop-Down Menus
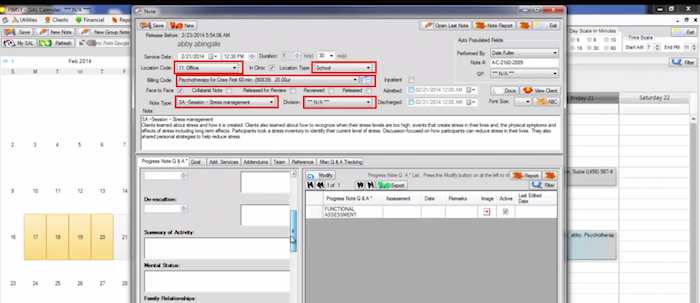

HOW IT WORKS: Drop-down menus are boxes that allow users to choose a value from a list or from a series of nested lists. Lists are hidden until the user clicks on, or hovers over, a particular value.
These can be incorporated in several different parts of the progress note where there is a finite amount of common answer options, such as service date and location data.
The screenshot above highlights several drop-down menus that are used throughout the progress note template. Information such as location code/type, billing code, note type and division has been entered in a drop-down menu so users can easily change it by selecting from pre-populated lists.
KEY BENEFITS: It’s ideal to place drop-down menus in any part of your note requiring basic information that can be templated in a list of limited-answer options. This time-saving measure makes data entry more efficient without crowding the interface. What’s more, most EHR systems allow you to choose your own menu answer options (e.g., specific locations or staff names).
Radio Buttons
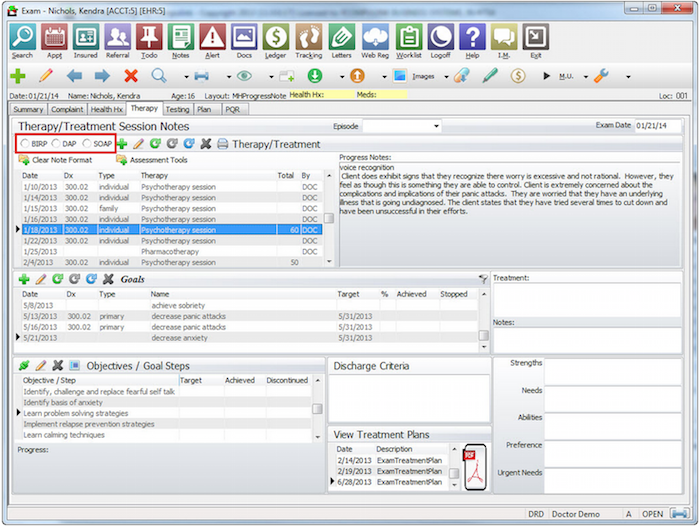

HOW IT WORKS: Radio buttons are used to select a single answer in a multiple-choice arrangement. Users can simply scroll over the circle next to their selection and click on it. These are usually incorporated at the start of progress notes to capture necessary information that only has a few answer options.
For example, in the screenshot above, the clinician is able to quickly choose the progress note format they’d like to enter. The options are:
BIRP (Behavior – Intervention – Response – Plan)
DAP (Data – Assessment – Plan)
SOAP (Subjective – Objective – Assessment – Plan)
KEY BENEFITS: Radio buttons should be used in sections of your progress note that call for straightforward data with very limited answer options. These may include note format, as shown in the example above, or assessment questions that require a “yes” or “no” answer.
Check Boxes


CareLogic Enterprise EHR by Qualifacts
HOW IT WORKS: There are two key points to know about this feature:
Check boxes are small boxes that can be selected with a checkmark to indicate an answer to a question, or to confirm whether a statement is applicable.
Check boxes are usually incorporated in sections of the progress note that relate to patient assessments or treatment plans.
The screenshot above shows a fictional patient’s progress note. The screen with the check boxes on the left represents all of the active treatment-plan goals for that client.
These are incorporated into the note so that the clinician can check off which goals, objectives and/or interventions were worked on or addressed during a particular session.
KEY BENEFITS: Check boxes prove valuable when your note requires you to update the status on a specific patient goal or to answer a series of “yes” or “no” questions.
This tool enables clinicians to spend more time engaging with patients, because they can simply tick off boxes to standard assessment questions instead of writing the answers out in full.
Open Text
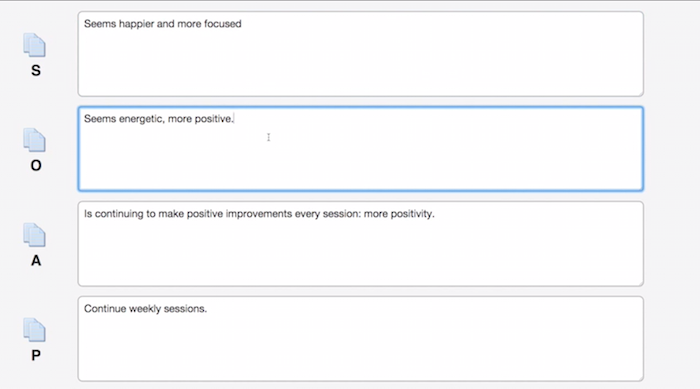

HOW IT WORKS: Open text fields allow clinicians to type in free-form entries without being restricted by pre-populated answer options. These can either comprise the entire progress note, or can be incorporated as an extra or optional section.
Depending on the system you purchase, these fields can be automatically populated so clinicians only have to add or subtract changes to the text from a previous session (shown in the screenshot above). Otherwise, open text fields can come completely blank so clinicians can type assessments from scratch.
KEY BENEFITS: Practices that need a greater deal of flexibility than templates may allow can benefit from incorporating open text fields as part of their notes template. Unstructured data like this usually allows clinicians to capture greater levels of detail per patient encounter.
Which Software Vendors Offer These Tools?
Most EHR systems on our list of top software products for mental health professionals offer the functionality described above to help you optimize progress notes for mental health care.
However, the variety of data-entry tools available and your ability to choose how they’re placed in your progress note templates may differ from product to product. Some vendors may even charge extra fees for personalized templates.
It’s important to determine how each of these tools align with your existing workflow, so you should consult with individual vendors to see if their software fits your needs and budget.
If you want some assistance creating a shortlist of products, reach out to our medical software advisors at (844) 686-5616 for a free consultation. In addition, you can also view top mental health software included in our latest FrontRunners for Mental Health.