HealthClaimsXG
No reviews yet
Overview
About HealthClaimsXG
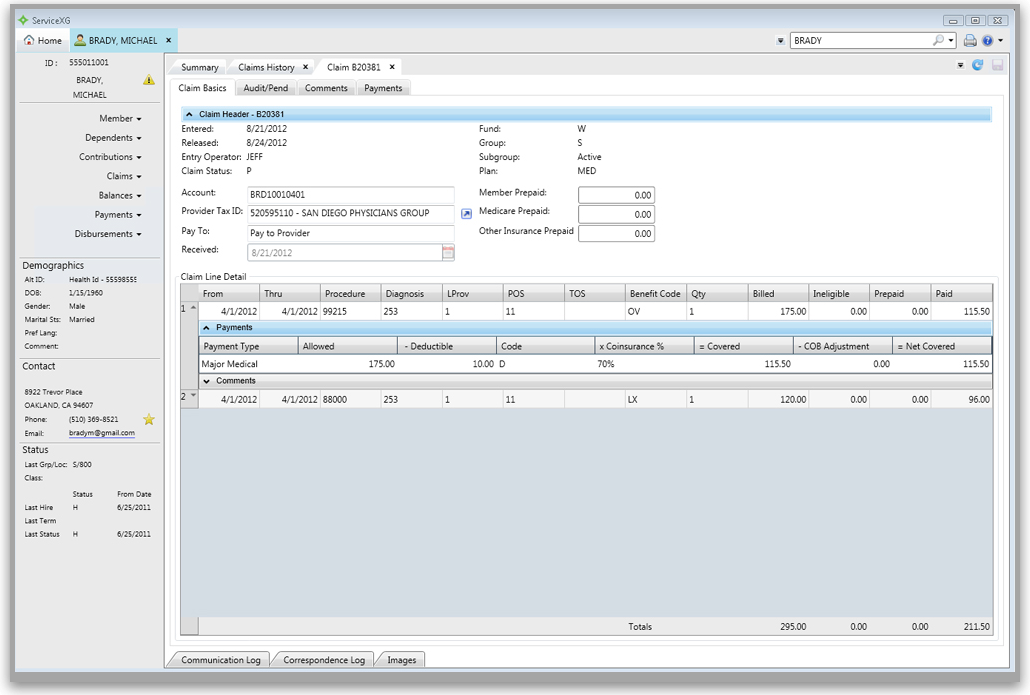
HealthClaimsXG from basys is a hybrid human resources management (HRM) solution that helps businesses to automate health benefits administration through by processing health care claims. The solution can either be deployed on-premise or hosted in the cloud.
HealthClaimsXG supports multiple claim types, including medical, dental, vision and short-term disability. A configurable auto-adjudication engine allows for batch processing, with user-defined audit capabilities and reporting tools available for users to manipulate data and control costs. There is also functionality for subrogation and case management that helps users to manage a large number of clients.
HealthClaimsXG supports integration with HRAs, HSAs and FSAs for billing purposes. It also integrates w...
HealthClaimsXG Pricing
Free trial:
Not Available
Free version:
Not Available
Other Top Recommended Human Resources Software
Be the first to review HealthClaimsXG
Share your thoughts with other users.




