Best Construction Categories
Best Facilities Management Categories
Best Human Resources Categories
Best Legal Management Categories
Best Manufacturing Categories
Best Medical Categories
Best Property Management Categories
Get 1-on-1 advice in 15 minutes. It's free.

Josh P.

How Much Does Medical Billing Software Cost? A Guide for Small Practices
Medical billing software costs vary widely, and small practices often struggle to understand what they should budget for.
Why is it complicated? Pricing depends on factors such as practice size, claim volume, deployment model, and whether the system includes tools like scheduling, reporting, or patient billing.
Why it matters: Small practices need clear cost expectations to avoid overspending and to choose a system that supports accurate claim submission, faster reimbursements, and fewer administrative bottlenecks.
Why you should read on: This guide breaks down common pricing models, typical cost ranges, and the features that influence price so small practices can make informed decisions before investing in a new medical billing tool.
Software vs. outsourced billing services
Medical billing software refers to applications you purchase to handle your billing in-house. Outsourced billing services, on the other hand, involve another company handling your billing tasks for you.
To avoid confusion, here’s a straightforward breakdown of how they compare:
Category | Medical billing software | Outsourced billing services |
|---|---|---|
Features | Billing platform, coding tools, claims management, and reporting | Full-service claims submission, follow-up, and denial management |
Cost structure | Subscription, per-claim fee, or one-time license cost | Usually, the service collects a percentage of the collection (4%–10%) |
Control level | Full control in-house | High dependency on the vendor |
Pros | Lower long-term cost and customizable workflows | Less administrative burden and fewer staffing needs |
Cons | Requires training & staff capacity | More expensive long-term, less transparency |
How is medical billing software priced?
Medical billing software is typically offered through several common pricing models. Each model affects how practices pay for the system and how costs scale with usage. Here are the primary pricing structures used by vendors:
Features that can increase cost
Claim scrubbing. This involves automatically checking insurance claims for errors or formatting issues before they get submitted to insurance firms.
Coding assistance. Some systems can suggest codes based on the documentation you present, come with built-in reference libraries, or use AI to analyze clinical notes and then recommend codes.
Reporting dashboards. Detailed dashboards can display important information, such as submitted claims, the number of days a payment has been in accounts receivable, or revenue per visit.
Additional integration capabilities. Some vendors may offer integrations with electronic health records (EHRs) or customer relationship management (CRM) systems.
User-based factors
Licensed user counts
Per‑provider models that charge separate fees for each clinician
Volume‑based tiers tied to claim counts or usage thresholds
Deployment type
Your deployment approach also affects cost:
Cloud‑based systems typically charge a recurring monthly subscription fee.
On‑premise systems often involve a large upfront license fee plus periodic maintenance fees.
Maintenance and upgrade needs vary. On‑premise systems may require internal IT time, while cloud systems typically include updates.
What are the different types of medical billing software pricing models?
Vendors tend to offer one or more of these pricing models:
Perpetual license: A one‑time software purchase that grants long‑term use of the system. Practices may still pay ongoing maintenance or update fees.
Tiered plans: Vendors offer multiple plan levels with varying feature sets. Higher tiers include more capabilities, and pricing increases accordingly.
Subscription fee: A recurring monthly or annual payment. Costs usually vary based on the number of users, locations, or included features.
Free or freemium software: Some vendors offer a basic version of their tools at no cost. Additional capabilities, higher claim limits, or support may require a paid upgrade.
Custom pricing: Larger practices or organizations with complex billing needs may receive a custom quote based on patient volume, locations, or advanced revenue cycle requirements.
Note: It’s essential to confirm with your software provider whether they offer free upgrades with a perpetual license purchase. If the software no longer works on a newer operating system (OS), some vendors may force you to pay for a brand-new version that’s compatible with your current OS.
Common subscription pricing tiers for medical billing software
Most medical billing systems follow a subscription model. Vendors typically charge either a per‑user monthly fee or a flat monthly practice fee, and pricing generally increases as claim volume, user count, or feature needs grow. Based on common market patterns, subscription plans for medical billing software typically fall into three tiers: entry‑level, mid‑tier, and high‑end.
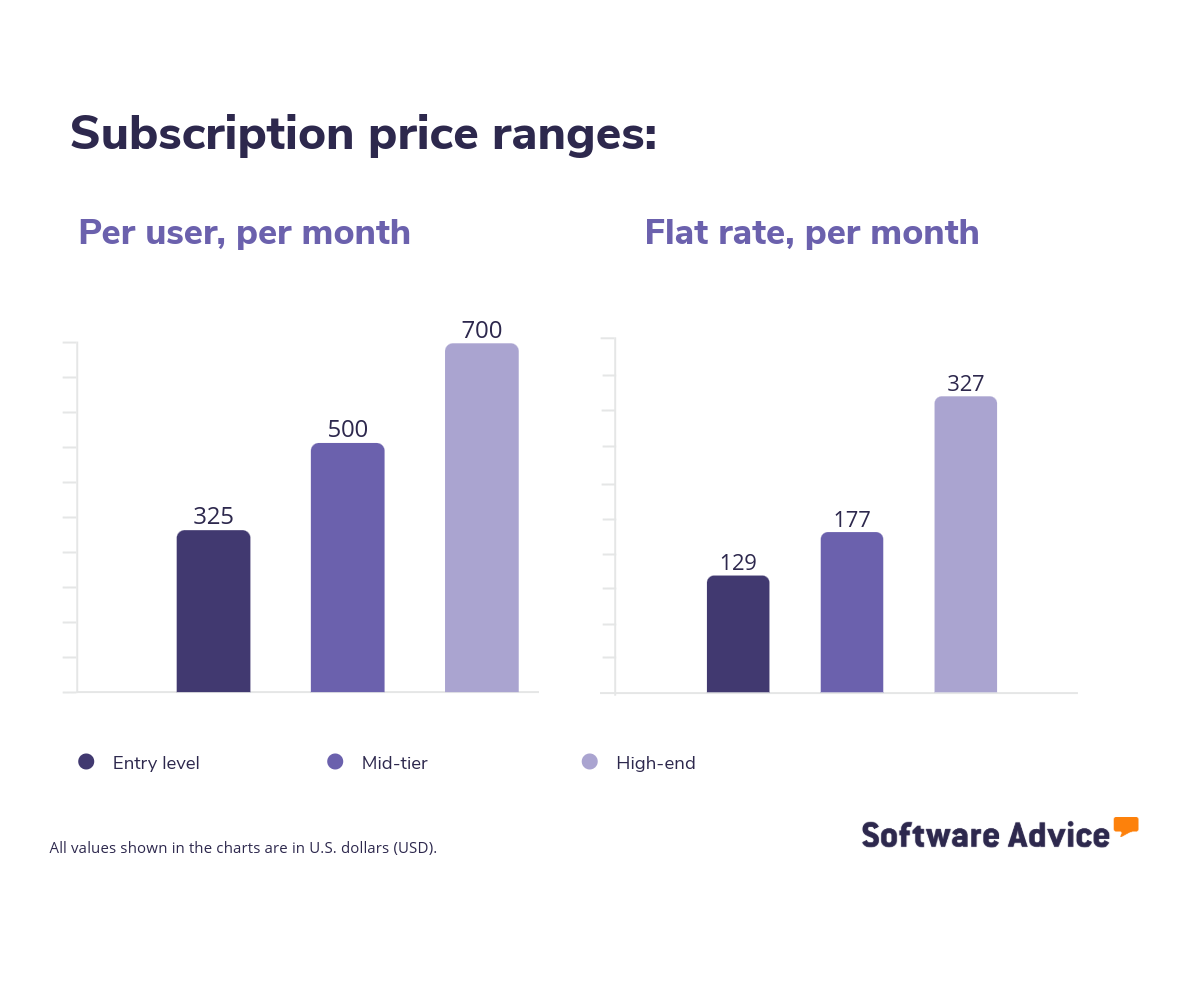
Entry‑level plans
These plans usually include the essential billing functions—claim submission, basic code lookup, and simple reporting. Entry‑level subscriptions commonly start around $325 per user per month or $129 per month for flat‑rate plans. They are often suitable for solo providers or small clinics with lower claim volumes.
Mid‑tier plans
Mid‑tier plans offer added capabilities such as claim scrubbing, payment posting tools, denial tracking, and integrations with electronic health record (EHR) systems. Typical pricing ranges from $500 per user per month to $177 per user per month for flat‑rate packages. These plans are a fit for practices that need more automation and visibility across the billing cycle.
High‑end plans
High‑end subscriptions include more advanced revenue cycle management (RCM) tools, analytics dashboards, multi‑location support, and broader integration options. Pricing generally falls around $700 per user per month or $327 per month for flat‑rate plans. These plans tend to support practices with higher claim volumes or more complex billing requirements.
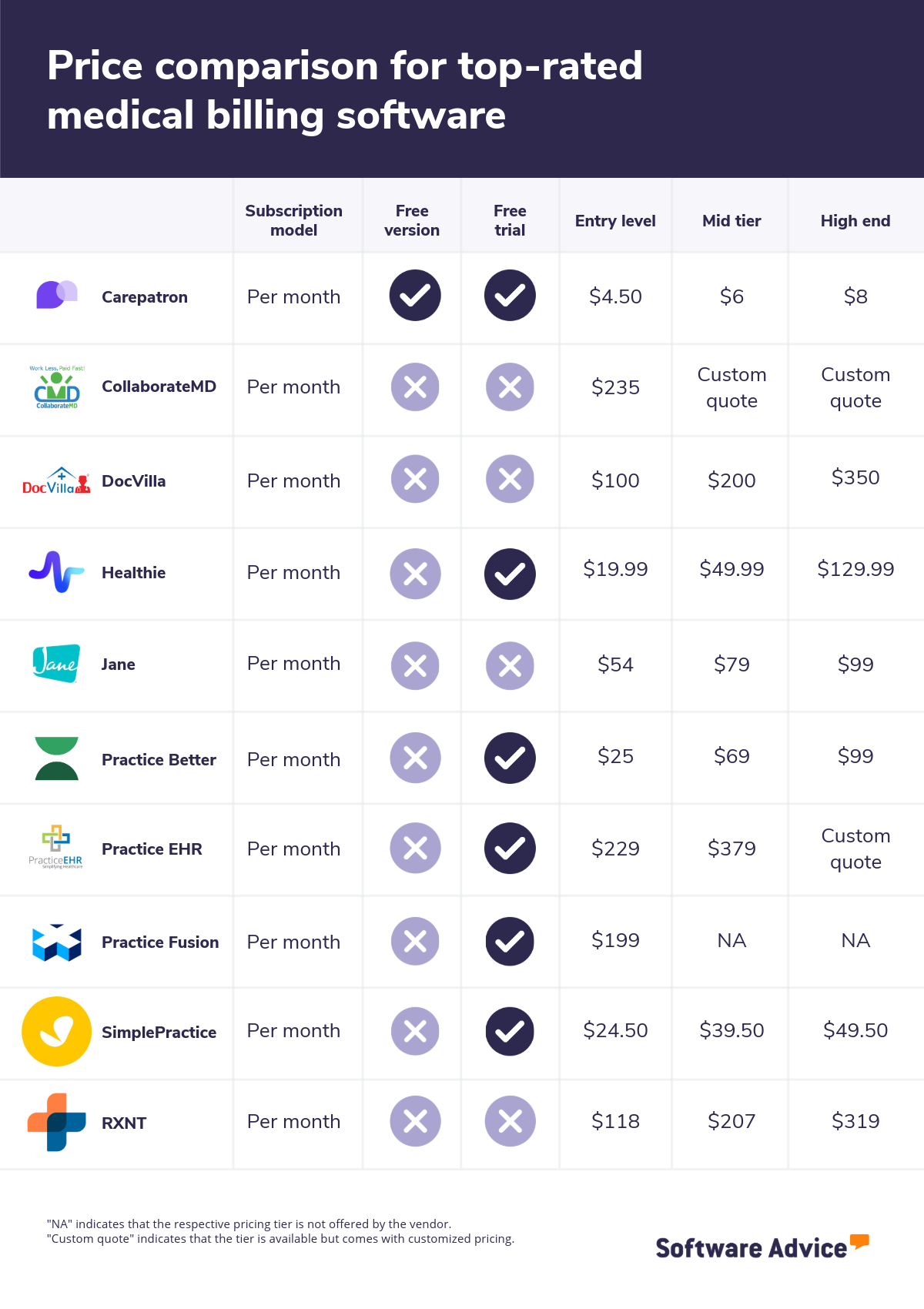
For reference, below is a snapshot of the prices for the most reviewed medical billing solutions, including subscription pricing plans. These products are taken from the most recent Software Advice FrontRunners report for medical billing software.
Cost comparison for top-rated medical billing software 2026
What are the upfront and recurring costs of medical billing software?
Upfront costs are those you pay before using the software, and they can be provided by the supplier or incurred as internal expenses. On the other hand, recurring costs occur regularly or are associated with services, features, or user add-ons.
Upfront costs may include:
Onboarding fees charged by the provider for helping you get set up
A flat software licensing fee you pay one time
Purchasing or configuring workstations or servers
Costs for data migration
Charges for staff training
Recurring costs involve:
Monthly or annual subscriptions
Support and maintenance charges
Charges for obtaining additional user licenses
Performing updates, which is common for on-premise installations
Pricing model breakdown
Pricing model | Upfront costs | Recurring costs |
|---|---|---|
Subscription | Low (sometimes $0) | Monthly/annual subscription |
Perpetual (on-premise) | High | Annual maintenance fees |
Free/freemium | None | Add-ons, transaction fees, and clearinghouse fees |
Hidden costs
While hidden costs may vary from one provider to another, some of the most common behind-the-scenes costs to look out for include:
Extra charges for data storage. You may be allotted a certain amount of data and end up incurring additional charges if you exceed that limit.
Premium support. It’s essential to understand the type of support included with your plan, as you may need to pay additional charges for on-demand or priority assistance.
Claims that exceed your monthly limit. If you pay based on the number of claims you process, you may end up getting hit with additional expenses if you cross a certain threshold.
What are the additional fees associated with medical billing software?
Vendors often charge extra fees—some required for billing, others tied to add‑on services, such as:
Clearinghouse fees. A clearinghouse is a service positioned between your practice and the insurance payer. They check claims for errors, convert them to the correct electronic format, such as ANSI 837, and perform other tasks.
Electronic remittance advice fees. These break down which claims were paid, denied, or adjusted, and the insurance payer may charge a fee for them.
Patient statement fees. A provider may charge you a fee for giving you patient statements about their billing history or balances.
Credit card or online payment fees. These typically come straight from your credit card company or online payment processing service.
How to find the right medical billing software price range
Getting your price range just right adds long-term sustainability to your billing ops. Here are some tips for aligning pricing with your budget and requirements:
Compare each option’s features to your needs. There may be some features you absolutely need, such as integration with an existing CRM, and those you could get by without, such as AI-powered coding assistance.
Factor in the pricing commitment. Do you want to be locked in for a year or longer, or do you like the option to opt out each month? Review the fine print of your contract to determine if there are any early termination penalties.
Check user limits. You have to compare the cost of adding users to your projected billing staff size.
Common questions to ask before choosing a pricing plan
Is there a free trial?
Many vendors offer a free trial of around 14 to 30 days.
Are long-term contracts mandatory?
Some providers require you to sign up for at least a year.
Is there an open-source version available?
Open-source software can be less expensive or free and highly customizable.
Pre-implementation checklist for medical billing software
Before committing to an implementation, there are a few boxes you need to check off:
Check the budget fit. The pricing structure fits within your monthly or annual budget without forcing trade-offs that strain finances over time.
Look out for hidden costs. Make sure there are no surprise fees—such as strict user limits or usage caps—that your team could easily exceed as workflows scale.
Ensure support costs are included. Confirm that the customer support offered with your plan is sufficient for your needs and already accounted for in your budget, rather than billed as an unexpected add‑on.
Make sure you get the required billing features. The software should include essential tools such as claims management, coding assistance, and denial tracking, so you’re not paying extra for core functionality.
Ensure system integrations. The application should integrate with the tools you already rely on, such as CRM or EHR software, reducing manual work and data silos.
Avoid common pitfalls. Make sure you’re not choosing a tool based on price alone, locking into a long contract with exit penalties, or settling for limited role‑based access that restricts how your team works.
Survey methodology
*The products in this guide qualified for the most recent FrontRunners for medical billing software and were highly rated by users. Only products with publicly available pricing information were included in this table. We summarized publicly available pricing sources, including vendor websites, as of January 2026, starting with the lowest monthly pricing (excluding annual discounts) for packages that include the core functionality for a software category. We list pricing for more advanced packages (per user, when available) that include the core software feature(s). Your company’s needs may differ, and final pricing may vary.