Best Construction Categories
Best Facilities Management Categories
Best Human Resources Categories
Best Legal Management Categories
Best Manufacturing Categories
Best Medical Categories
Best Property Management Categories
Get 1-on-1 advice in 15 minutes. It's free.

Josh P.

Top 6 Medical Billing Systems With AI‑Enabled Features
Medical practices use AI‑enabled billing tools to capture documentation, identify coding patterns, flag errors, and accelerate reimbursement cycles through natural language processing, machine learning, and predictive analytics. AI medical billing software also supports practices by predicting denial risks, surfacing undercoded services, and learning from past claims outcomes.
Why it matters: Many practices still struggle to balance AI adoption with daily billing workflows, especially when accuracy checks, data privacy, and staff trust are involved.
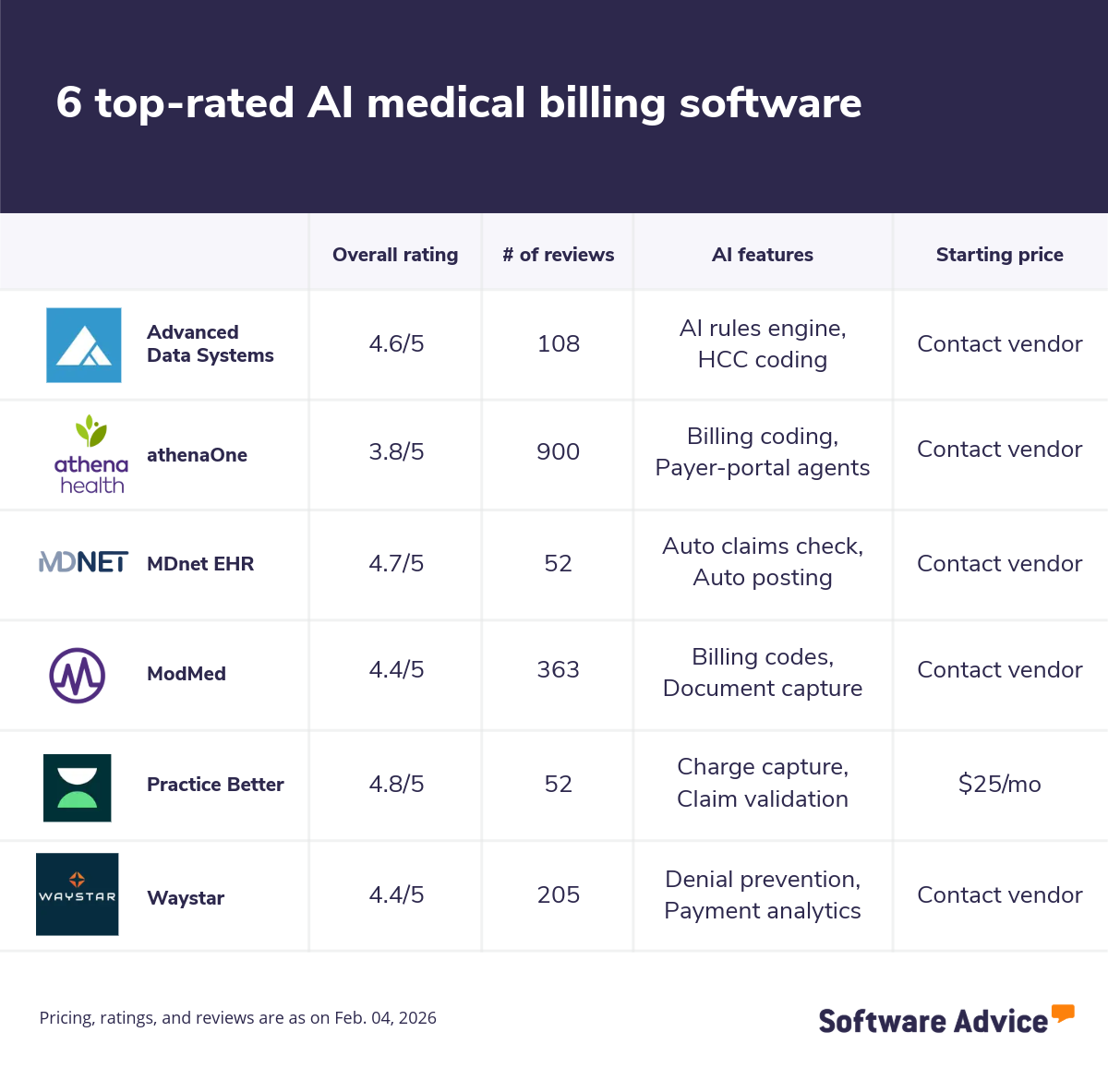
Below is a list of the 6 top‑rated AI medical billing software, sorted alphabetically, based on verified user reviews and our research team's analysis. These tools cater to medical billing needs, including claims submission, coding assistance, denial management, documentation capture, and payment posting.
Advanced Data Systems
Advanced Data Systems uses MedicsScribe AI for voice‑to‑text data input and real‑time clinical capture. It surfaces denial‑risk alerts before claims go out and supports cleaner claim submission by identifying potential issues early. These AI‑supported capabilities allow practices to streamline coding, maintain cleaner claims, and capture encounter details more efficiently.
AI-enabled medical billing features*:
AI rules engine: Analyze claims for potential errors or over‑coding, providing alerts before submission so that practices can correct issues and avoid rework.
HCC coding: Use automated coding guidance within billing workflows, including risk‑adjusted categories such as hierarchical condition coding (HCC).
Clinical documentation: Capture provider speech in real time and convert it into structured clinical documentation inside the patient record.
Customer support options: Chat, FAQs, help center, knowledge base, and user community
Who should consider Advanced Data Systems’ AI capabilities?
Small multispecialty practices with frequent claim edits may benefit from Advanced Data Systems’ AI rules engine. It flags coding and claim‑level issues before submission to help reduce denials and maintain steadier cash flow.
Starting price: Available upon request from the vendor
athenaOne
athenaOne is an AI‑native revenue cycle platform that learns from large volumes of real claims and payer policy updates. In practice, that means the system can interpret insurance card images to pick the right coverage, apply continuously refreshed payer rules to prepare cleaner claims, and delegate portal lookups to AI agents, so fewer tasks depend on manual checks and copy‑paste work.
AI-enabled medical billing features*:
Billing coding and documentation improvement: Recommend procedure codes and identify documentation gaps in real time during clinical note creation.
AI payer‑portal agents: Automatically search payer websites for policy changes, prior authorization updates, and claim status, reducing follow‑ups and accelerating authorization‑to‑payment cycles.
Automated insurance selection: Analyze insurance card images and select the correct coverage automatically, reducing insurance‑related denials and claim holds.
Customer support options: Chat, help center, and knowledge base
Who should consider athenaOne’s AI capabilities?
athenaOne suits practices with complex payer mixes or heavy front‑office workloads. Its AI agents automate insurance checks, apply payer rules, and reduce manual portal lookups, helping front‑office and billing teams maintain cleaner claims.
Starting price: Available upon request from the vendor
Pro tip
Prioritize AI features that help your billing team reduce manual checks, spot errors before claims go out, and shorten the time between service and reimbursement.
MDnet EHR
MDnet EHR uses AI to review and correct claims in real time, detect potential denial risks, and recommend resolution steps so billing teams can act before revenue is delayed. With automated denial detection, claim‑level insights, and policy‑aware billing logic, MDnet EHR helps practices maintain cleaner claims and streamline their financial workflows.
AI-enabled medical billing features*:
Patient account management: Use AI within the revenue cycle module to analyze patient billing data, identify discrepancies, and guide corrective actions.
Auto claims check: Review claims in real time, identify errors, missing data, or payer‑specific issues before submission to flag or correct problems.
Auto posting: Automate denial detection and posting decisions by analyzing payer responses and suggesting resolution steps.
Customer support options: Chat, call, email, help center, and knowledge base.
Who should consider MDnet EHR’s AI capabilities?
Billing teams with heavy follow‑up workloads (e.g., multi‑specialty groups or billing firms managing multiple payers) may get the most value from MDnet EHR’s AI claims follow‑up agent and AI‑assisted patient billing. The platform uses agentic AI to pursue claim status, surface next‑best actions, and handle patient billing questions, helping reduce time spent on phone calls and in portals while keeping A/R moving.
Starting price: Available upon request from the vendor
ModMed
ModMed’s AI focuses on turning clinical documentation into accurate billing inputs by suggesting codes tied to specialty‑specific terminology, surfacing billing‑relevant details during charting, and reducing the administrative steps that often lead to incomplete or inaccurate claims. Its AI‑driven scribing and coding intelligence help practices capture revenue more consistently by connecting what happens in the exam room with what needs to be billed.
AI-enabled medical billing features*:
Billing codes: Translate specialty‑specific clinical language into suggested billing codes to support cleaner claims and reduce missed charge opportunities.
Documentation capture (ModMed Scribe 2.0): Convert natural conversation into structured documentation using specialty‑trained models, producing complete and bill‑ready notes that reduce post‑visit coding gaps.
Claims denial assessment: Evaluate why claims were denied by comparing documentation, coding, and payer requirements; highlighting patterns, such as coding inconsistencies or documentation gaps; and providing actionable insights to address root causes.
Customer support options: Call, chat, webinar, and knowledge base
Who should consider ModMed’s AI capabilities?
Teams seeking to reduce documentation‑driven coding gaps and ensure that nuanced clinical language (e.g., dermatology findings, orthopedic exam details, ophthalmology diagnostics) automatically flows into bill‑ready codes will benefit most from ModMed’s AI capabilities. Its specialty‑trained AI and Scribe 2.0 help capture clinically specific details that generic billing tools often miss.
Starting price: Available upon request from the vendor
Practice Better
Practice Better’s AI enhances medical billing by automating charge capture, reducing coding errors, and identifying claim issues before submission. It uses machine learning to extract billing codes from clinical notes, validate claims for compliance, and reduce real-time denial risk. These capabilities help practices accelerate reimbursements and reduce manual billing work.
AI-enabled medical billing features*:
Charge capture: Extract billing codes directly from clinical documentation, minimizing manual coding and improving accuracy.
Claim validation: Use machine learning to check claims for compliance issues, missing details, and potential errors before submission.
Denial prevention: Flag patterns and issues likely to cause payer denials, helping practices correct them early.
Customer support options: Help center, knowledge base, and user community
Who should consider Practice Better’s AI capabilities?
Providers who want to reduce claim denials using smart claim validation may benefit most from Practice Better, as its AI proactively detects errors and compliance gaps—helping smaller clinics submit cleaner claims without additional billing staff.
Starting price: $25 per month
Billing cycle: Annual
Pro tip
Choose front‑end AI tools that verify coverage accurately and back‑end AI automations that guide follow‑up, so your practice can prevent avoidable rework and keep claims moving.
Waystar
Waystar’s Altitude AI automates medical billing, claim workflows, prioritizes tasks, and reduces errors from eligibility through denial appeals. The suite combines predictive models, agentic assistants, and generative AI to autonomously identify appropriate insurance coverage across the revenue cycle, fix bad payer data before submission, and generate payer‑ready content (e.g., appeal letters) and next‑best actions directly within claim workflows.
AI-enabled medical billing features*:
AI denial prevention and appeal generation: Identify high‑impact pre‑submission fixes and auto‑generate appeal letters for denied claims.
Predictive denial and payment analytics: Anticipate outcomes, forecast trends, and surface at‑risk claims so teams can focus effort where it moves A/R fastest.
Work prioritization with AI assistants: Rank and route billing tasks (e.g., follow‑ups, underpayment review) to improve staff throughput and focus on high‑value actions.
Customer support options: Call, webinar, and knowledge base
Who should consider Waystar’s AI capabilities?
Waystar fits practices dealing with frequent coverage mismatches or documentation‑driven delays. Its AI identifies correct insurance data, applies pre‑submission fixes, and generates payer‑ready appeals for denied claims.
Starting price: Available upon request from the vendor
What are the benefits of using medical billing software with AI capabilities?
AI medical billing systems improve billing accuracy, reduce rework, and accelerate reimbursement. These benefits reflect common capabilities across top AI‑enabled billing platforms.
Benefit | Description |
|---|---|
Increased efficiency | Automates repetitive billing tasks such as charge capture, coding, and claim preparation, reducing manual workload and speeding up the billing cycle. |
Fewer claim denials | Uses machine learning to detect errors, compliance issues, and missing details before submission, helping practices prevent denials in advance. |
Improved billing accuracy | Extracts accurate billing codes directly from clinical notes and documentation, reducing risks of miscoding and claim rework. |
Better financial visibility | AI‑powered dashboards provide insights into payment trends, aging A/R, and cash flow, supporting stronger financial decision‑making. |
Automated follow‑ups | Tracks unpaid claims, flags outstanding balances, and prompts timely follow‑ups to improve collection speed and reduce A/R days. |
How much does AI medical billing software cost?
AI‑enabled medical billing platforms vary in price depending on features, automation depth, practice size, and included EHR or practice‑management tools. Based on available pricing from reputable medical billing software listings, the following pricing patterns are typical.
Free trials: Many AI‑enabled billing platforms offer free trials ranging from 7 to 30 days, allowing users to test features before subscribing. Trials commonly include access to core billing workflows or limited AI features.
Free versions: Some platforms offer permanently free plans for small practices, but these free tiers typically exclude advanced AI billing features such as automated coding or denial prediction. Basic free plans are usually limited to scheduling or documentation tools.
Entry‑level plans: Start at $7 per user, per month, and include basic billing tools with limited automation.
Mid-tier plans: Typically range from $10 to $30+ per user per month, adding AI‑enabled features such as automated coding assistance, claim validation, and analytics. These plans suit growing practices that need more automation and revenue‑cycle visibility.
High-end plans: Higher‑tier pricing often applies to platforms with advanced AI capabilities (e.g., denial prediction, automated follow‑ups, integrated EHR + billing intelligence). These plans suit multi‑provider practices or clinics with complex billing needs.
Hidden costs associated with AI medical billing software
Besides the software license, additional costs may include:
Training: Additional onboarding or workflow training may incur extra fees.
Third-party integrations: While many AI billing tools offer integrations with popular third-party services and platforms, some integrations may incur additional costs, such as subscription fees or usage-based pricing.
Data storage: Digital storage is included in most AI medical billing tools’ subscription plans. However, lengthy files may require additional storage, which the software vendors may charge for.
Frequently asked questions when selecting AI medical billing software
Here are some common questions to ask software vendors:
What training data does the AI rely on, and how is accuracy monitored? Ask vendors what data trains their system (your past claims, de‑identified multi‑customer data, payer rule libraries, and specialty‑specific examples) and how often clinical code sets (ICD‑10‑CM for diagnoses) and CPT/HCPCS for procedures are refreshed. The makeup and freshness of the training data, and how accuracy is measured, directly influence coding precision, denial rates, and staff trust in the system. If the model isn’t tuned to your specialties or monitored after go‑live, you risk more rework instead of less.
What security and compliance safeguards are in place? Billing data contains protected health information; weak safeguards expose you to breach risk, regulatory penalties, and reputational damage. Strong controls ensure patient privacy and reduce legal and operational risk. Confirm the vendor will sign a Business Associate Agreement and comply with HIPAA. Ask for independent security attestations (such as SOC 2 Type II or ISO 27001), encryption standards (TLS in transit, AES‑256 at rest), role‑based access with single sign‑on and multi‑factor authentication, and full audit logs. If outside AI services are used, they require private, HIPAA‑eligible endpoints, clear data‑residency (where your data is stored and processed), a complete list of sub‑processors, and the option to keep your patient data out of any shared model training.
How customizable are the AI rules and automation workflows? Customization lets you reflect local payer policies and operational realities; without it, the AI may apply generic rules that miss revenue opportunities or trigger unnecessary rework. Determine whether you can tailor rules by payer (edits, documentation needs, prior‑auth nuances) and set confidence thresholds that govern automation (for instance, auto‑apply high‑confidence suggestions, queue medium‑confidence items, and reject low ones).
Are AI features included in the base price or offered as add‑ons? Transparent packaging prevents surprise costs and helps you model the total cost of ownership; it also ensures you’re not locked out of critical automation behind unexpected add‑on pricing. Ask the vendor to map each AI feature to a plan and a pricing unit (per user, per provider, per claim, or per number of AI calls), and to disclose usage caps, overage rates, and one‑time setup or integration fees. Identify which capabilities, such as autonomous coding, denial prediction, or appeal drafting, require premium tiers.
Survey methodology
To be considered for this list, products had to:
Have at least 20 unique product reviews published on Software Advice within the past two years, with an average rating of 4.0 or higher (as of Feb. 04, 2026).
Meet our market definition for medical billing software: “Medical billing software provides features that support coding, claims processing, payment posting, or revenue cycle activities commonly used by healthcare organizations.
Show evidence of offering AI capabilities as demonstrated by publicly available sources, such as the vendor’s website.
For the section titled “How much does AI medical billing software cost?”, only products with publicly available pricing information and AI features, as of Feb. 04, 2026, were considered for pricing calculations.
*Our research team identified these features from vendor websites (as of Feb. 04, 2026) based on their analysis of what users find valuable in or expect from AI-enabled medical billing software. This list is not exhaustive. For additional capabilities, refer to the vendor's website.
Editorial Independence: We select and rank products based on an objective methodology developed by our research team. While some vendors may pay us when they receive web traffic or leads, this does not influence our methodology.