Find the best Medical Billing Software
Compare Products
Showing 1 - 20 of 207 products
Sort by
Reviews: Sorts listings by the number of user reviews we have published, greatest to least.
Sponsored: Sorts listings by software vendors running active bidding campaigns, from the highest to lowest bid. Vendors who have paid for placement have a ‘Visit Website’ button, whereas unpaid vendors have a ‘Learn More’ button.
Avg Rating: Sorts listings by overall star rating based on user reviews, highest to lowest.
A to Z: Sorts listings by product name from A to Z.
athenaOne
athenaOne
FrontRunners 2024
The athenaOne Suite which includes athenaCollector a revenue cycle management solution and athenaClinials an EHR (electronic health records) recently ranked #1 in 2023 Best in KLAS for athenaClinials Ambulatory EMR for 11-75 physi...Read more about athenaOne
RXNT
RXNT
FrontRunners 2024
RXNT’s cloud-based, ONC-certified medical software—Billing, Practice Management, EHR, and more—improves clinical outcomes & revenue cycle management. Simple, transparent pricing includes free setup and training, free data transfer...Read more about RXNT
DrChrono
DrChrono
FrontRunners 2024
DrChrono’s iPad and iPhone compatible EHR and medical billing platform allows medical practices and healthcare providers to manage patient intake, patient care, clinical charting, billing and revenue cycle management. It includes ...Read more about DrChrono
ChartLogic EHR
ChartLogic EHR
ChartLogic offers an ambulatory EHR suite that includes electronic medical record, practice management, revenue cycle management, e-prescribing and patient portal. The solution caters to primary care, surgical care and other compl...Read more about ChartLogic EHR
Talk with us for a free
15-minute consultationSoftware Advice is free because vendors pay us when they receive sales opportunities.
This allows us to provide comprehensive software lists and an advisor service at no cost to you.
This allows us to provide comprehensive software lists and an advisor service at no cost to you.
Meet Eric, a software expert who has helped 1,534 companies select the right product for their needs.
Talk with us for a free
15-minute consultationSoftware Advice is free because vendors pay us when they receive sales opportunities.
This allows us to provide comprehensive software lists and an advisor service at no cost to you.
This allows us to provide comprehensive software lists and an advisor service at no cost to you.
Tell us more about your business and an advisor will reach out with a list of software recommendations customized for your specific needs.
STEP 1 OF 4
How many doctors are in your organization?
MDnet EHR
MDnet EHR
FrontRunners 2024
Enable Healthcare presents a state-of-the-art electronic health records solution designed to transform the way doctors and providers manage patient data. Our AI-powered charting, powered by EnableAssist, revolutionizes charting ef...Read more about MDnet EHR
Compulink Healthcare Solutions
Compulink Healthcare Solutions
FrontRunners 2024
Compulink Advantage is an all-in-one database EHR solution for specialty practices such as optometry, ophthalmology, orthopaedics, ENT, mental health, podiatry, and more. Available cloud-based or server, Advantage includes smart f...Read more about Compulink Healthcare Solutions
Nextech EHR & PM
Nextech EHR & PM
For more than 20 years, Nextech has provided a full-featured EMR and Practice Management solution within a single database. This system is a fit for dermatologists, plastic surgeons, ophthalmologists, and physicians, and is used b...Read more about Nextech EHR & PM
ModMed
ModMed
FrontRunners 2024
ModMed, also known as Modernizing Medicine®, is an award-winning software company that places doctors and patients at the center of care through an intelligent, specialty-specific cloud platform. Services include electronic health...Read more about ModMed
Practice EHR
Practice EHR
FrontRunners 2024
Practice EHR, a medical practice management software, was developed to accommodate the needs of small to mid-size businesses. The platform is customizable to internal medicine practices, chiropractors, physical therapists, family ...Read more about Practice EHR
AllegianceMD
AllegianceMD
AllegianceMD is a cloud-based medical software system that is designed to serve the needs of small and midsize practices, as well as ambulatory surgery centers. The solution includes practice management functionality for billing a...Read more about AllegianceMD
Nexus EHR
Nexus EHR
Nexus EHR is an ONC Certified 2015 Edition Cures Update cloud-based ambulatory EHR and PM platform. It is designed for small to midsize practices and various specialties including orthopedics, neurology, podiatry, cardiology, gene...Read more about Nexus EHR
CharmHealth
CharmHealth
FrontRunners 2024
CharmHealth is a MU certified, cloud-based EHR, Practice Management and Medical Billing solution that helps healthcare organizations ranging from large multi-specialty groups to small independent medical offices function efficient...Read more about CharmHealth
NextGen Office
NextGen Office
FrontRunners 2024
NextGen Office is an award-winning, cloud-based, clinical and billing solution designed for smaller, independent practices (≤ 10 providers). This all-in-one, full-service solution includes specialty-specific EHR content, an easy-t...Read more about NextGen Office
WRS Health
WRS Health
More than just a cloud-based EHR & Practice Management software. At WRS Health, our commitment to helping physicians find balance in their roles, as healer, business owner, and human being, informs everything we do. That’s why ...Read more about WRS Health
CollaborateMD
CollaborateMD
CollaborateMD is a medical billing and practice management solution that helps practices and billing services of all sizes automate and streamline billing and coding processes. The system was designed to be both comprehensive and ...Read more about CollaborateMD
DocVilla
DocVilla
DocVilla is a HIPAA-compliant Cloud-based software for medical practices. DocVilla offers integrated EHR (Electronic Health Records), EMR (Electronic Medical Records), Telemedicine, Electronic Prescriptions (eRx), EPCS (Electronic...Read more about DocVilla
Azalea Health
Azalea Health
Azalea provides cloud-based electronic health records (EHR), practice management (PM), revenue cycle management (RCM) and telehealth solutions for ambulatory and hospital care settings. Azalea is suitable for community and rural h...Read more about Azalea Health
NextGen Enterprise
NextGen Enterprise
NextGen Healthcare provides scalable, integrated solutions and professional services to help your practice administer excellent care and operate your business more efficiently. We serve medium to large enterprise-level ambulatory ...Read more about NextGen Enterprise
Net Health
Net Health
Net Health Therapy for Hospitals – Outpatient is cloud-based rehab therapy documentation, scheduling and practice management software designed specifically for hospital outpatient settings. A fully-integrated solution, Net Health...Read more about Net Health
AdvancedMD Billing Services
AdvancedMD Billing Services
AdvancedMD is a medical office software suite with cloud-based, integrated physician-patient workflow solutions including: practice management/medical billing, electronic health records, telemedicine, patient engagement, practice ...Read more about AdvancedMD Billing Services
Popular Comparisons
Buyers Guide
Last Updated: March 16, 2023What is medical billing software?
Medical billing software is used by healthcare providers to automate their manual billing tasks, such as verifying patients’ insurance, processing and submitting claims, processing payments, and following up on denied claims. The software helps providers increase their collections by avoiding repetitive and cumbersome administrative tasks.
The software can be purchased either as a standalone system; as an integrated part of an electronic health records (EHR) solution; or as an integrated part of a practice management suite.
Medical billing software automates repetitive and error-prone billing tasks. It helps medical offices:
Increase collections
Code claims properly
Verify patients’ insurance coverage
Post payments and EOBs
Provide reports on collections and rejections
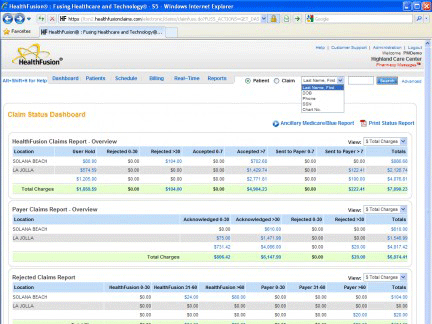
Claim Status Dashboard in MediTouch by HealthFusion
There are hundreds of computerized medical billing systems on the market and they range from functionally simple to very sophisticated. The most basic systems help providers generate paper statements based on demographics and billing codes input by the user. Additionally, medical office billing software allows providers to submit claims electronically, scrub claims, post payments, pull advanced reports and more.
In this guide we discuss the following:
What is Medical Billing Software?
Common Features of Medical Billing Software
Benefits of Medical Billing Software
Popular Medical Billing Software Comparisons
Common Features of Medical Billing Software
When comparing different medical billing software, it’s helpful to have an understanding of the common features offered with this software. Here are some of the features you can typically expect in a medical billing system:
Claims processing | Automates the process of creating, submitting, tracking, and processing medical insurance claims in order to collect payment from providers. |
Claims scrubbing | Run claims through an auditing procedure before submitting them to find and correct any errors in coding. This feature helps reduce denied or rejected claims and increase approval rates. |
Insurance verification | Checks patient insurance eligibility ahead of appointments to ensure procedures and services will be covered by patient insurance. |
What Type of Buyer Are You?
Most practices we speak with match one of these common buyer types:
Inpatient care providers. This category of buyer includes hospitals and long-term care facilities that need to submit claims using UB-04 forms. This type of form typically requires a system designed for inpatient billing, although some outpatient healthcare billing software systems do have a module for UB-04 billing.
Outpatient care providers. This category is made up of the private practices that submit claims on the CMS-1500 forms. These buyers need to submit electronic claims to Medicare, Medicaid and private insurance companies using Medicare billing software/Medicaid billing software. Software needs do not vary much by size of organization, although larger organizations will need a more robust, scalable medical insurance billing software program.
Specialists. Specialists such as chiropractors, naturopathic doctors and mental health providers of varying designations typically see patients that pay directly via cash or credit card. Moreover, their patients typically do not submit many (if any) claims to insurance companies or government payers. As a result, these providers have more lightweight needs.
Outsourced billing services. These buyers are third-party companies that submit claims on behalf of providers. They are typically paid a percentage of collections by providers. They have similar functional requirements to their respective provider clients, but may require a very broad, flexible system if they bill for clients of varying specialties or types of care.
Integrated suite buyers. These buyers require billing functionality, but would rather implement one integrated suite for scheduling and EMR. Their vendor selections are often driven by the EMR functionality, since most integrated systems are differentiated by their EMR offering, not their billing modules.
Benefits and Potential Issues
Billing software is an integral part of the overall revenue cycle management process. Billing and other administrative tasks are notoriously paper-laden and cumbersome. A modern medical billing software system allows billers to be as efficient as possible at coding, submitting and following up on claims.
Moreover, staff will find that medical billing and coding software helps them code claims accurately to avoid errors. As a result, most providers find their collection rates increase when going from manually submitting claims to using medical claim software.
Finally, advanced reporting tools typically provide insights that are tough to gain without a medical billing solution. By collecting important data around claims and payers, such as which claims get rejected most often and which payers pay the slowest, providers can make data-driven decisions to improve collections.
Most practices and billing services we speak with face a common set of billing challenges, and consequently, they’re considering purchasing (or replacing) software to address those challenges. Here are common scenarios we often hear about during our phone consultations:
Transitioning from paper claims. Typically, solo or small practices are making the move from paper claims to an electronic system (though that is not always the case). They have a difficult time keeping track of patients and who owes what. They will implement medical billing software for the first time to reduce paperwork, track all data in a central place and improve efficiency overall.
Bringing billing in-house. Another common scenario, most practices choose to bring billing in house—as opposed to outsourcing to a third-party service—to cut costs, have more control of their billing and accounts receivable and get everything centrally located.
Replacing antiquated software. Finally, offices replacing their existing system do so because it’s outdated and expensive to maintain, it doesn’t meet their technical requirements (e.g., integration with electronic medical record software) or they have a difficult time using it. In this scenario, Web-based medical billing software is an attractive option because it’s modern and easy to use, costs less up front and updates automatically as vendors release new versions and enhancements.
Medical Coding Software
Many medical billing software solutions include functionality that enables HIPAA-compliant medical coding. Users can enter procedure and diagnosis codes and even look up codes online to find the correct ones. This capability allows users to file and track claims more easily and helps in the tracking of data over time. Many medical billing software solutions will also update codes automatically to ensure the accurate ones are always being used.
Costs and Return on Investment
The prices of medical billing software programs often depend on the application’s deployment model. On-premise systems will require upfront costs for licenses, servers and other necessary hardware, setup and training. Buyers of on-premise systems will also need to pay ongoing maintenance and support fees, which are typically 15-20 percent of the upfront licensing costs.
Software-as-a-Service (SaaS) applications typically require lower upfront costs and ongoing monthly fees that cover licensing, support and upgrades. Finally, there are free medical billing software options that are supported by alternative revenue streams, such as advertising.
Most buyers who have successfully implemented systems will be able to generate returns on their investments through improved accuracy of filings, improved billing efficiency, and subsequently, increased collections.
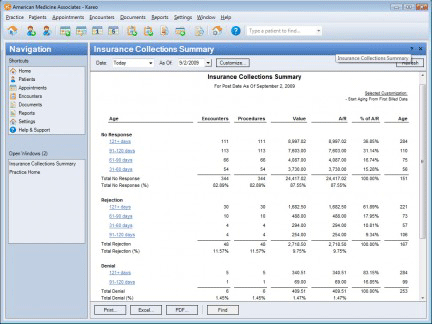
Collections Management in Kareo speeds payment
Important Considerations
Integrated suites vs. stand-alone billing solutions. Buyers will need to decide if they want to implement a standalone system, a system integrated with patient scheduling (typically called “practice management”) or a fully integrated billing, scheduling and electronic medical records (EMR) system. Many vendors such as AdvancedMD and NueMD offer all three options. Medical billing solutions have long been the only or primary applications used in many doctors’ offices, and they are usually the first systems new practices will implement. Despite government legislation requiring the adoption of EMRs, we still hear from many practices looking for standalone billing or practice management systems.
On-premise vs. Web-based. SaaS or Web-based medical billing systems have become very popular and comprise well over 50 percent of new solution sales. Low upfront costs, greater accessibility and little to no IT requirements are contributing factors to so many buyers preferring Web-based systems. Assuming buyers have reliable Internet access, we typically recommend they consider these programs.
Security. A primary concern we hear from buyers regards data security. Since medical billing involves the storage and transmission of so much sensitive patient data, buyers will want to make sure they implement a secure system. Vendors are well aware of this need and offer HIPAA-compliant systems.
User adoption. Usability tends to be more a function of the end user and how the system is configured than the medical claims software itself. Users with medical experience can typically adopt most systems quickly. Many complaints regarding usability tend to be related to setup and maintenance of servers and other hardware, not the applications themselves.







